Voices of U of U Health
What Will the “New Normal” of COVID-19 Look Like?
Two years into the COVID-19 pandemic, and fresh on the heels of the Omicron surge, it's clear that COVID-19 isn't going away any time soon. The virus will almost definitely continue to mutate, evolve, spread, recede, and then start the whole process all over again.
As we grapple with this "new normal," our governments, medical institutions, and—most importantly—each of us as individuals will have to learn from the past and be ready to adapt to the reality of ever-present COVID-19.
Will COVID-19 Be with Us Forever?

In the early stages of COVID-19, nations tried to contain and eradicate the strange new virus. Recommendations from health experts and governments changed at a dizzying pace, encompassing everything from lockdowns to mask mandates and social distancing. Scientists and pharmaceutical companies launched a breakneck race for a vaccine in hopes of eradicating the virus.
The emergence of vaccines offered hope that COVID-19 would wither away if it couldn't find enough hosts for it to incubate and spread.
But that hasn't happened. Despite lockdowns, COVID-19 spread. Despite the availability of vaccines, not everyone got vaccinated, allowing COVID-19 to spread and mutate into forms that can sicken even vaccinated people—though vaccines continue to be the best defense, greatly reducing severe illness, hospitalizations, and deaths when compared to those who aren’t vaccinated.
So, what does that mean for the future of COVID-19? It means that we're going to have to live with this virus for a long, long time. It won't always be a "pandemic." The average pandemic lasts two and a half to three years. That doesn't mean the virus goes away. Instead, what usually happens is that people move on socially before the disease ends.
Masking or Vaccines? What Will Stick Around the Longest?
It's tricky to use past pandemics as a guidepost for what to expect after this one. The most recent pandemic of a similar style was the 1918 flu. The world was much different then, with slower travel and fewer people on the planet.
After the 1918 flu pandemic, people abandoned masks within a few years. As COVID-19 sticks around, we likely won't see masking last forever. Widespread mask wearing will probably fall off sooner than it should.
We should still strive to use common sense when it comes to masks as part of the new normal. The mask issue has become unnecessarily polarized and political. On the individual level, some people refuse masks altogether. Others wear face masks all the time, even outside when no one's around. The best approach is somewhere in the middle.
You don't always have to wear masks outside when people are sparse, but it is still recommended to wear a mask in crowded situations.
One thing that probably will be a big part of life going forward is the regular booster shot. Periodic boosters, much like seasonal flu shots, will most likely be the norm, though we're not sure how frequently we'll need them.
We do know these vaccines are very safe. Getting vaccinated and boosted is certainly safer than catching COVID-19. The best advice is to get fully vaccinated and boosted if eligible, especially if you have risk factors. And if you do contract COVID-19, seek treatment right away. Treatments have been developed that are very effective at preventing hospitalizations in people.
Lessons Learned in Health Care and Society

In some ways, COVID-19 will be similar to the flu, in that it's seasonal. But in other ways, it's going to be much more severe. During the "mild" Omicron wave, we saw 2,500 deaths a day from the disease. In a bad flu year, we might see 50,000 deaths the entire season. Omicron beat that in a month.
Beyond immediate deaths, we will continue to see direct and indirect effects of COVID-19 for many years to come.
Many people who contracted COVID-19 will have to live with the effects. We have a huge number of patients who were debilitated from previous COVID-19 episodes. They will very likely end up in the hospital or ICU with even a mild respiratory illness. That's something we're going to be dealing with for a generation.
Because of hospital capacity and staffing during some of the heaviest days of the pandemic, many people did not get the regular health care they should. We're going to see ripple effects from that for the next few years.
Health care systems learned some valuable lessons. Building a strong team that can handle a constantly changing situation put us in a better situation than almost any other preparatory step. University of Utah Health made some critical decisions early on that helped us do well—these include keeping all of our staff and ensuring we had adequate PPE.
Biggest Lesson Learned? It's Up to Us to Determine Risk
We take risks all the time. Every time we get in a car, ride a bicycle, or leave our front door, we take a risk. We mitigate those risks by wearing seatbelts and bike helmets and looking both ways before crossing the street.
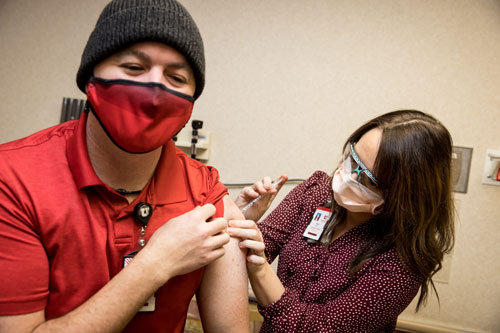
Living with COVID-19 is much the same. We'll need to be aware of the risks we're taking when going about our daily routine, and then work to mitigate those risks by getting vaccinations and boosters and masking when appropriate. These considerations will be omnipresent for people with compromised health or immune systems.
Risk awareness goes hand in hand with responsible media consumption. The news during the COVID-19 pandemic was often confusing. Things got worse when people got their information from unreliable news sources. Having access to reliable information is going to be critical for public and individual health.
People will need to have the skills to sort out reliable news from misinformation. With health news, people should go to their own doctor with their questions.
The biggest change we need to make and live with in the future is this: We'll have to think carefully about how our actions impact those around us.

