Voices of U of U Health
COVID-19 Research Showcases Strength Across Campus
As the pandemic began and it became clear it would be a worldwide health crisis unlike any of us had ever seen, University of Utah sprang into action. Researchers across campus were remarkably responsive and nimble: the first thing we did was make sure that our whole community was safe. Starting with widespread communication, we assessed levels of safety for every unit in 18 colleges, schools, and institutes across health sciences, main campus, and the innovation district.
Safety First
Safety was our first objective. Then, almost immediately, we pivoted to say, "How do we leverage this time?" Mainly to create an environment where our people could still keep moving forward on their research as much as possible, but also conduct what we called "impactful COVID research," which we prioritized during that time. We did that with a significant amount of seed-grant funding. We started with 56 seed-grant projects in diverse disciplines and studies across campus. Everybody stepped up: from the clinical research front to basic science investigation, to applied science, and solution-based initiatives across the entire university.
As of this month, the U is conducting more than 400 research projects related to COVID-19, to study the virus from all angles: from testing and vaccine trials to its impact on vulnerable communities and rates of domestic violence, to the social, psychological, and economical strains COVID-19 has on our society. Our research has appeared in more than 450 academic publications and has been cited more than 5,500 times. To finance the research, $1.3 million has come from U seed funding and $45 million from external funding, demonstrating strong confidence from local, national, and international agencies in our expertise.
Surveillance Testing
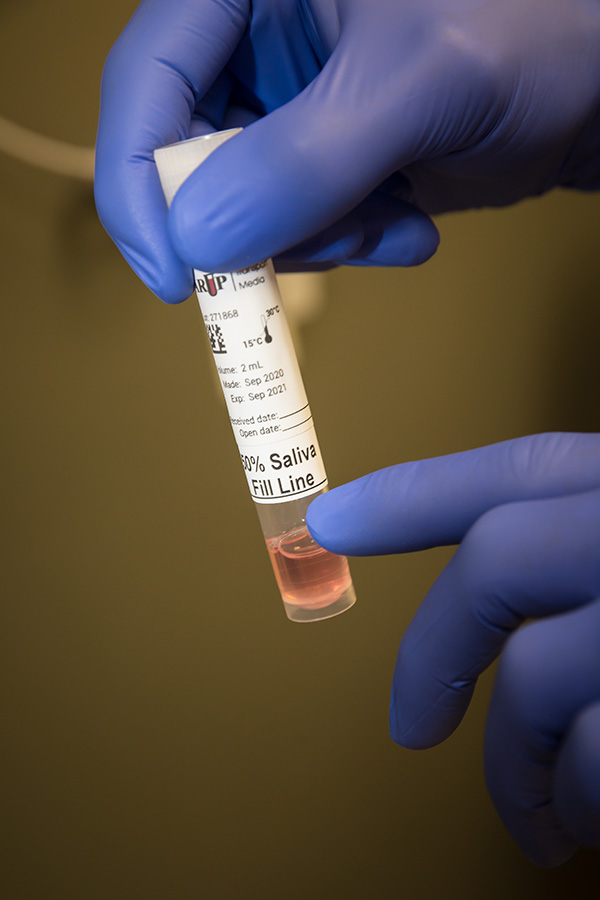
Our research expertise was put to use for the very practical purpose of keeping the campus running safely and efficiently. In January, we developed an asymptomatic testing capability so that all students, staff, and faculty can take highly accurate saliva tests even if they aren’t exhibiting symptoms. This asymptomatic testing, also known as surveillance testing, aims to find the people who feel well but have the virus, and could be unknowingly spreading it.
John Phillips, PhD, director of the Health Science Center (HSC) Core facilities leveraged the expertise and resources at the Core Labs to make this happen. We’re still heavily using this test because it also detects virus variants and has been used to monitor the prevalence of the Delta variant. The Core Labs have run 66,837 tests between January 11, 2021 and September 9, 2021, and its operation has been accurate and reliable. The test has now been extended to U-affiliated households. This important service is helping to keep our U campus and local communities safe.
Long-Term Implications
A key area of COVID-19 research for us has been long-term implications. One of the major things that we don't understand yet is what happens after a person is infected over the long haul? If a young person gets infected, is it going to be problematic for them in regards to heart disease or something else down the road? We have research teams focused on studying "long COVID-19" – people with one or more symptoms that have persisted for weeks or months after initial infection. Large grants are now submitted and they're already working on answering those questions in pilot studies. University of Utah Health has also opened a post-COVID-19 care clinic for so-called "long haul" patients. This clinic will work in collaboration with our researchers.
Associated Disease
There are a number of ongoing studies on infectious disease that were converted in rapid fashion to include COVID-19. Beth Middleton, MD, Con Yost, MD, and their teams are working on novel therapies. Their approach was rapidly adapted from a study of sepsis to address COVID-19 and acute respiratory distress syndrome (ARDS).
The researchers have a novel inhibitor that blocks so-called NETs (Neutrophil Extracellular Traps) from forming. These small structures develop during sepsis and block micro blood vessels, causing clotting. They found that this also happens in COVID-19 patients. Very quickly, they were able to start testing whether a NET inhibitor that they had been testing as a therapy for sepsis could similarly prevent COVID-19 from worsening in preclinical models.
Society and Behavior
COVID-19 infection is influenced, of course, by socio-economic factors and human behavior, two areas of additional research. Daniel Mendoza, PhD, and Tabitha Benney, PhD recently published a research study on how income, occupation, and neighborhood influence a person’s chance of getting COVID-19. They compiled statistics from Salt Lake City broken down by ZIP codes. The numbers clearly demonstrated that people who are less affluent got COVID-19 at a rate 10 times higher than other, more affluent residents. During the 2020 lockdown, the residents of affluent areas were able to stay at home more than residents of the least affluent ZIP codes. The data suggests that “essential worker” occupations, which are typically held by minority populations, placed people at greater risk for contracting COVID-19. Research led by Fares Quedan, PhD, Tiana Rogers, PhD, and Charles Rogers, PhD, found a similar pattern. They showed that Black Americans across the country are more likely than Whites to hold essential worker positions and die from COVID-19.
Life Circumstances
Researchers on campus are also studying the impacts of COVID-19 on life circumstances. For example, what is the psychological impact of social isolation, on older adults in assisted living facilities and patients in the ICU? There are major implications not just for people isolated but for everybody in their lives. We need to remember that science is more than metrics and analytics-- there is also the human piece. That piece can have a large influence on many aspects of health.
We think of COVID-19 research at the University of Utah as being service-oriented work that benefits our local and global communities. We're looking at the impact of COVID-19 on air quality, socioeconomics, how it impacts underrepresented groups, the implications on healthcare both short-term and long-term and so much more. One of the great things about the university is that we have strengths in so many different areas, so we can look at this problem from multiple angles. That's pretty remarkable.
We have already learned an enormous amount, but our understanding will only grow broader and deeper over the months and years to come. Our research community has risen to the occasion during this time of need. We do this work to make a difference in the lives of the people around us.

