Voices of U of U Health
Here to Stay: the Era of Telehealth
Virtual health care is here to stay. Many believe the era of telehealth was launched by the coronavirus pandemic. It wasn’t, but the health crisis certainly accelerated it. Prior to the pandemic, two percent of University of Utah Health providers had seen patients virtually—now, 90 percent have. From March 2020 to March 2021, our providers held 400,000 virtual telehealth sessions. That amounts to between 6,000 and 8,000 sessions a week.
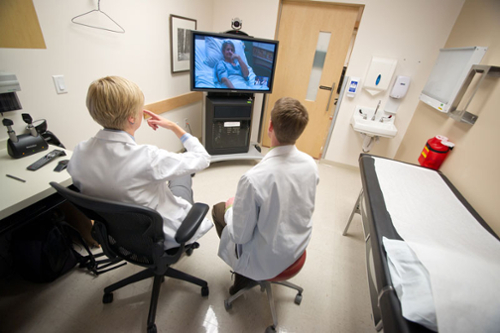
Telehealth will continue to evolve. It already involves more than live transmission of a patient’s face onto a provider’s device while the patient describes his or her state of health and asks questions. As diagnostics continue to improve, patients will be able to do more within their own homes. Wearable medical devices are increasingly integrated with remote care delivery. Remote labs continue to emerge, changing how patients monitor their health. Think of swabs that patients collect in the comfort of home and drop into a mailbox for analysis. This exists for genetic testing companies like 23andMe. We did it with COVID-19 tests. Coronavirus testing advanced quite rapidly so that someone at home could do a self-swab and send it back to a central lab.
For more complex lab diagnostics, imagine the day when a lab technician comes to your home to collect samples for testing or perform imaging tests like an x-ray. The idea is to flip the supply chain upside down: instead of the patient coming to the hospital, lab, or imaging center, why not the hospital, lab, or imaging center going to the patient?
Easier Access
The premise of all these things is making health care more convenient, easier to access, and ultra-consumer-centered. Delivery in the home, or wherever it may be convenient for the patient, is a rapidly expanding trend. Video visits are just one component of it. Certain visits still need hands-on evaluation, often with a video component. From my perspective as an orthopaedist, we had to develop a structure for telehealth sessions to be effective. We now have a short video we send to patients ahead of time that tells them the multiple steps they should take before treatment. For a new patient appointment, I need the patient to make certain videos and take certain photographs of themselves to send in, before I see them virtually. My colleagues and I intend to streamline virtual visits even more because it's incredibly cost-effective and time-effective for the patient.
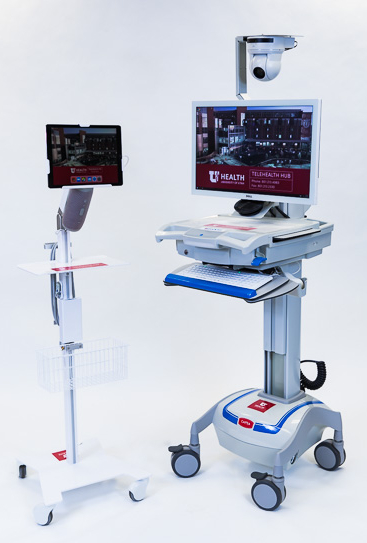
Telehealth also means better access to care and treatment at U of U Health for our patient base geographically spread across the Mountain West and beyond. We have one of the most rural populations of a major academic medical center anywhere in the country. Virtual care gives us a chance to reach out, talk to, and evaluate patients across broad geography without them needing to leave their home or burn carbon fuels. It gets us even closer to University of Utah Health’s goal of providing our regional population with access to world-class patient-centered care.
Still Not for Everyone
With telehealth’s initial success and great potential, it’s still not for everyone—nor effective for every condition. Many patients remain skeptical about virtual visits, thinking their physician may not get an accurate picture or full understanding of their health issue. There are also patients who just find comfort and reassurance from in-person conversations. We need to give patients choice. As long as it is clinically appropriate, telehealth works well—especially when we match the right circumstances to a patient’s preference.
Our data shows that what’s wanted is as varied as our patient populations. A core group of more digitally literate patients quickly recognized the benefits of virtual care. Most of these patients connect to us with their smartphones. They are motivated to learn quickly because digital technology connects with their physician—and helps them bring in family members from dispersed locations to participate in health care visits. Yet there's a huge swath of our patient population that hasn’t had enough digital experience to be comfortable talking device to device.
The telehealth option is increasingly widespread. It's not just at U of U Health, an academic health organization with state-of-the-art digital equipment, where the reconfigured world of patient care is underway. Traditional health care business models of all sizes are expanding home-based clinical care. Coalitions have formed among health care groups to support policy changes that designate the home as a site of clinical service.
With vaccinations and the number of COVID cases falling during the last couple months, there's been an appropriate decrease in virtual care within our system. But it has not returned to pre-COVID levels. It is here to stay. So our mission in approaching the new normal is to pivot and be especially strategic about virtual care to ensure that we use it to meet the needs of our patients. Whenever possible, we also want to offer the deep resources of our academic tertiary health care system. We need to maintain exceptional value with high standards of quality and experience for patients and providers.

